Live-stream
Session: Orthognathic and TMJ Track: Hot-off-the-Press and Abstract Session
GP2d - Quality Assurance Protocol for In-house Orthognathic Splint Fabrication
Thursday, September 21, 2023
3:40 PM - 3:50 PM PDT
Location: Room 20A, San Diego Convention Center

Talal Beidas
Resident
Virginia Commonwealth University
Houston, Texas
Yotom A. Rabinowitz, DDS
Assistant Program Director, Assistant Professor
Virginia Commonwealth University
Richmond, Virginia
Presenting Author(s)
Co-Author(s)
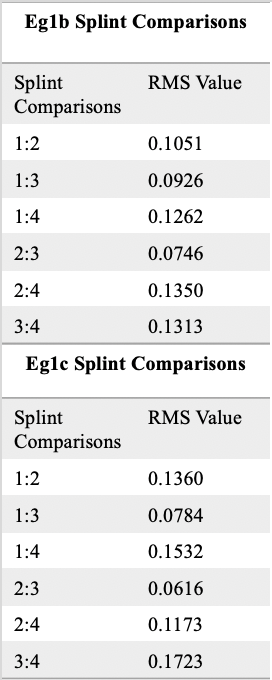
Abstract: Outsourcing virtual surgery planning and splint fabrication has become the standard in the field of orthognathic surgery. However, point-of-care planning and printing may reduce working time and improve efficiency (1). In-house protocols have already been proposed for single jaw surgery at select centers with success (2). As more clinicians adopt this model, regulatory bodies are likely to enforce quality and manufacturing standards. The layering process during stereolithography can result with baseline printing errors in orthognathic splints that are not well documented. In light of impending regulatory concerns, the purpose of this study is to propose an in-house quality assurance protocol for point-of-care 3D printers. This method would account for documentable baseline errors involved with in-house printing, scanning, designing, reproducibility, and machine discrepancies. We performed an in-vitro pilot study in an academic clinical setting. Outsourced orthognathic splint STL files were both 3D-printed (four copies) with resin and also milled with zirconia, which is a process devoid of potential layering errors present in printing. Control group 1 (cg1) consisted of a standard-shaped orthognathic splint. Experimental group 1a (eg1a) consisted of cg1 milled and sintered on a PrograMill7 from Ivoclar (figure 1). Experimental group 1b (eg1b) included cg1 printed on a Formlabs 3B+ printer, a FDA-compliant machine. Experimental group 1c (eg1c) included cg1 printed on a Phrozen 4K printer, an open-platform printer used in the clinic. Experimental groups were scanned on a 3Shape E4 scanner to generate a STL file. STL files were then uploaded and trimmed on 3Matics by Materialise. They were then superimposed on the control STL, and surface area overlap was analyzed via root mean square (RMS) value. Statistical analysis was performed with SASv9.4. A two one-sided t-test at the 0.05 level was used to test for equivalence of RMS between the Phrozen and Formlabs printers. Average RMS value for a milled splint was 0.10. This accounted for scanning error alone. RMS for the milled group was subtracted from the printed groups to calculate the pure printing error. On average, the RMS for the Phrozen printer was 0.02 units higher than the Formlabs, but the two were deemed equivalent within the bounds of +/- 0.20 (p < 0.0001) (figure 2). Results from the TOST method demonstrated equivalence bounds of (-0.06, 0.01) for Formlab versus Phrozen. The average RMS for pairs of reprinted splints was 0.111 (95% CI: [0.085, 0.136]) for the Formlab printer and 0.115 (95% CI: [0.075, 0.165]) for the Phrozen printer. Overall, the average RMS for replicates was 0.115 and did not differ significantly from the observed scanning error of 0.11 (p=0.5954) (figure 3). By employing this protocol, we were able to quantify potential manufacturing errors, and provide evidence of a highly accurate in-house printing process on multiple machines. Splints printed in the clinic exhibited acceptable baseline printing errors in reproducible fashion, nearly replicating their origin STL files. Documenting these values and protocols may prove useful to maintain compliance with regulatory standards, which are currently unclear but evolving. We recommend that clinics operating point-of-care 3D technologies for orthognathic surgery develop similar quality testing algorithms.
1. Steinhuber T, Brunold S, Gartner C, Offermanns V, Ulmer H, Ploder O. Is virtual surgical planning in Orthognathic surgery faster than conventional planning? A time and workflow analysis of an office-based workflow for single- and double-jaw surgery. J Oral Maxillofac Surg. 2018;76:397–407.
2. Mascarenhas W, Makhoul N. Efficient in-house 3D printing of an orthognathic splint for single-jaw cases. Int. J. Oral Maxillofac. Surg. 2021, 50, 1075–1077.
Figure 1
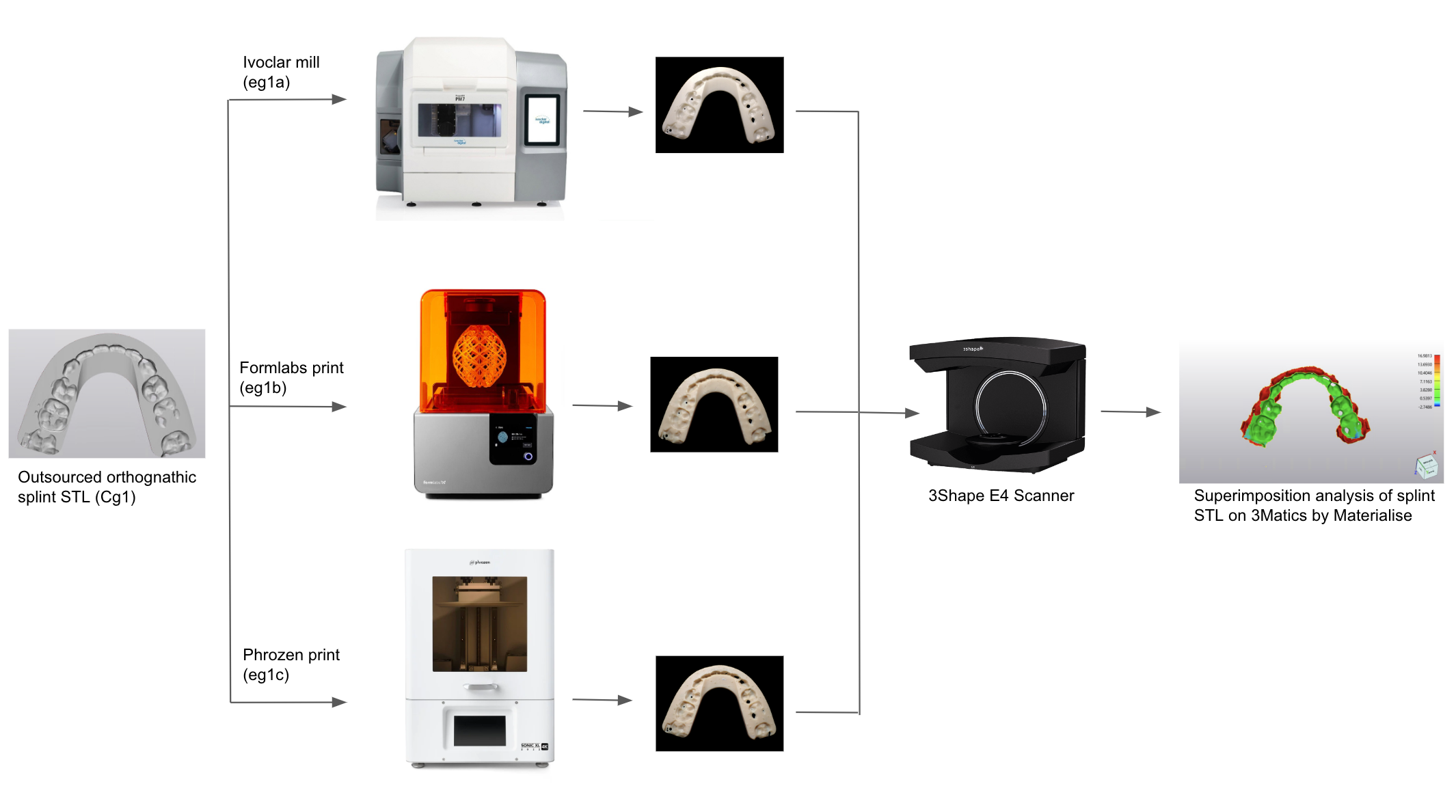
Figure 2
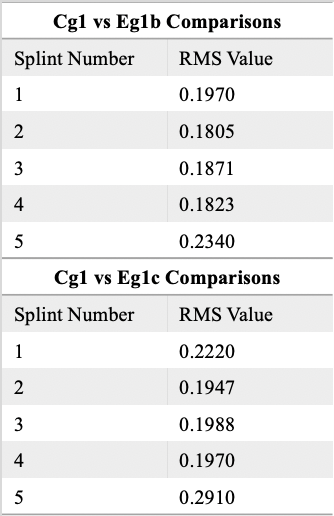
Figure 3
1. Steinhuber T, Brunold S, Gartner C, Offermanns V, Ulmer H, Ploder O. Is virtual surgical planning in Orthognathic surgery faster than conventional planning? A time and workflow analysis of an office-based workflow for single- and double-jaw surgery. J Oral Maxillofac Surg. 2018;76:397–407.
2. Mascarenhas W, Makhoul N. Efficient in-house 3D printing of an orthognathic splint for single-jaw cases. Int. J. Oral Maxillofac. Surg. 2021, 50, 1075–1077.
Figure 1

Figure 2

Figure 3



